Repair of Perineal Lacerations
Perineal lacerations should be sutured immediately after the delivery of the placenta. The sooner the lacerations are repaired, the smaller the danger of infection. Suturing is not recommended until the placenta has been delivered because manual invasion of the uterus may become necessary if complications develop in the placental stage of labor.
All rules of asepsis should be observed in the repair of perineal lacerations. The operative field and surgeon’s arms should be cleansed and scrubbed as for obstetrical operation.
A catgut suture should be placed on the upper angle of the wound in the vaginal wall; the ends of the thread should be pulled upwards by forceps. Two forceps are used to clamp the wound edges in the region where the vaginal mucosa converts into the perineal skin. Using the ligature and two clamps, the wound is opened, dried up, and the character of laceration studied. The torn off wound edges should be removed.
The first degree of perineum lacerations are repaired by placing catgut sutures on the vaginal mucosa, and then silk sutures on the perineal skin. Sutures should be spaced at 1 cm intervals. The needle should pass under the entire wound surface; otherwise slits will remain where blood will accumulate to interfere with healing. The wound should be ligated so that its edges tightly contact each other. In such case the wound would be healing.
The order of repairing the second degree perineal lacerations is as follows: the upper angle of the wound is first sutured, and then the lacerated perineal muscles are repaired by several buried catgut sutures (the sutures should not involve the skin or mucosa). The vaginal mucosa should then be sutured up to the posterior fourchette. The ligature ends (except at the posterior fourchette suture) should be cut off. The latter suture is pulled upward to facilitate suturing of the perineal skin. The perineal skin should be sutured with a silk thread and its ends cut off. (Metal staples can also be used.) The sutured wound should be treated with an iodine tincture (Fig.212, 213, 214, 215).
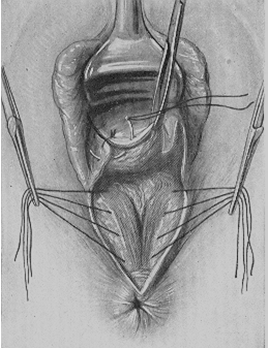
Fig. 212. Closing the vaginal sulci
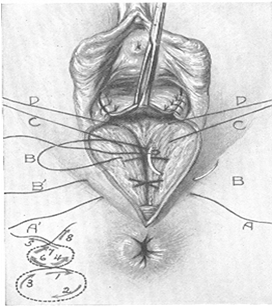
Fig. 213. Repairing of the perineal muscles
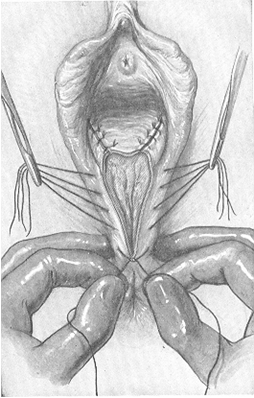
Fig. 214. Closing the wound
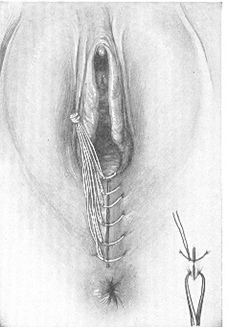
Fig. 215. Completion of the operation
In repairing the third degree perineal lacerations, the injured wall of the rectum should first be sutured (Fig. 216). The separated ends of the lacerated rectal sphincter should then be identified and sutured (Fig. 217). Next the order is the same as in repairing the second degree perineal lacerations.
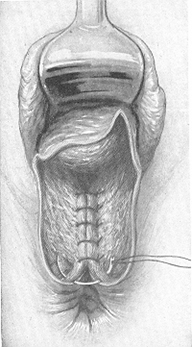
Fig. 216. Repairing of the 3rd degree of perineal laceration: Suturing of the rectal mucosa
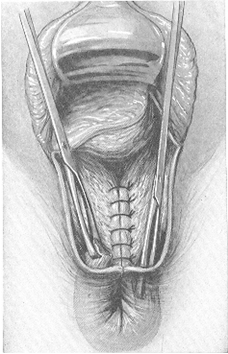
Fig. 217. Reaching down into the bottom of the sphincter ani
The postoperative care in perineal lacerations consists in keeping the sutures clean. Sterile gauze should be used to cover the wound (renewed at 3-4 hour intervals). The wound may, however, be kept without gauze covers. The suture should be washed off 3–4 times a day, after which it should be dried up by sterile pad and treated with antiseptic drugs. The suture should also be dried up after washing the external genitalia after defecation or urination. Usual regimen should be recommended for puerpera, they are only forbidden to sit.
The patient should be recommended a light diet: sweet tea, broth, and other digestible food.
In cases with the third degree perineal lacerations 2-3 capsules of loperamid should be given to the puerpera every day during six days in order to keep away stools. Approximately on the sixth day of postpartum period castor oil may be given or an oil enema may be administered.
Silk thread should be removed in 5 or 6 days. The patient is allowed to rise on the following day after removal of the sutures.
Lacerations in the region of the clitoris and lips are often accompanied by marked bleeding. The laceration of the cavernous body may cause a considerable loss of blood. All lacerations should be repaired. When the clitoral area is repaired, a metal catheter should be inserted into the urethra to preclude its involvement in the suture.
Lacerations of the Vagina. Insufficient distensibility of the vaginal walls, infantilism, operative parturition, delivery by extended vertex, large fetal head, etc. are among the causes of vaginal lacerations. The lower third of the vagina is commonly lacerated (along with laceration of the perineum).
Lacerations of the vagina are usually revealed by specular inspection and sutured by catgut. Lacerations of the lower third of the vagina may be repaired with separation of its walls by the fingers of the left hand.
Lacerations of the Vagina. Insufficient distensibility of the vaginal walls, infantilism, operative parturition, delivery by extended vertex, large fetal head, etc. are among the causes of vaginal lacerations. The lower third of the vagina is commonly lacerated (along with laceration of the perineum).
Lacerations of the vagina are usually revealed by specular inspection and sutured by catgut. Lacerations of the lower third of the vagina may be repaired with separation of its walls by the fingers of the left hand.
Hematoma of the vulva and vaginal walls. Blood vessels may rupture during delivery and the subcutaneous connective tissue of the external genitalia or the vaginal submucosa will be effused with the blood, while the overlying coat remains intact. The skin and the mucosa overlying thus formed hematoma become red-blue and if much blood accumulates in the tumor, the tissues become strained and painful.
Treatment of small hematomas is expectant. An ice bag is first placed on the affected area but later a careful treatment with physiotherapeutic warmth should be given. If hematoma swells rapidly, the skin should be incised, the hematoma emptied, and the broken vessel tied up. The incised site should then be repaired.
Date added: 2022-12-25; views: 782;
