Bleedings During Placental Stage of Labor and in Puerperal Period
Bleedins During Placental Stage of Labor. Complications in the placental stage of labor are more frequent than during the dilation and expulsive stages. The most frequent and dangerous complication of the placental stage is bleeding.
Hemorrhage is normal for the placental stage of labor and a blood loss of approximately 0.5% of body weight during the separation and delivery of the placenta is considered physiological. There is a significant contraction of the uterine musculature during the placental stage of labor. This is followed by (a) separation of the placenta and expulsion of the separated placenta (afterbirth) and (b) compression of the bleeding uterine vessels and cessation of the hemorrhage. If contractions of the uterus are weak, the normal separation of the placenta is upset.
The placenta fails to separate completely, but until the entire placenta is separated the uterus does not contract and the vessels at the site of the separated placenta continue bleeding. If the placenta has separated from the uterine wall but is retained inside the uterus, bleeding develops as well. The uterus fails to contract adequately until the placenta is expelled from it, and the vessels continue bleeding because of lack of compression.
Therefore, two normal mechanisms of cessation of hemorrhage in the 3rd stage of labor are distinguished: contractions of the uterine muscles and increased coagulability of blood, the latter being characteristic of this term of gestational process.
Hemorrhage in the placental period may also be caused by:
· Failure of the process of placenta separation from the uterine wall and its expulsion;
· Laceration of soft tissues of the reproductive tract: cervix, vagina, and perineum.
Hemorrhages due to Failed Separation and Expulsion of the Placenta (Afterbirth). Adherent placenta. Total and partial adherences of the placenta are distinguished. The main characteristic sign of the adherent placenta is an underdeveloped spongy layer (Fig. 190, 191) of the decidual membrane. It leads to the partial separation of the placenta, partial contractions of the myometrium fibres, resulting in hemorrhages. Partial adherence of the placenta is the cause of inevitable bleeding in the placental stage.
Total adherence of the placenta, as a rule, is not characterized by bleeding. It is characterized by absence of placental separation during 30 minutes and more, which is an indication for the manual removing. And during this removing bleeding happens, as a rule; this bleeding is arrested when the uterus is emptied and contracted.
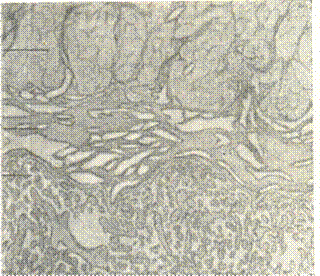
Fig. 190. Normally developed spongy layer of the decidual membrane
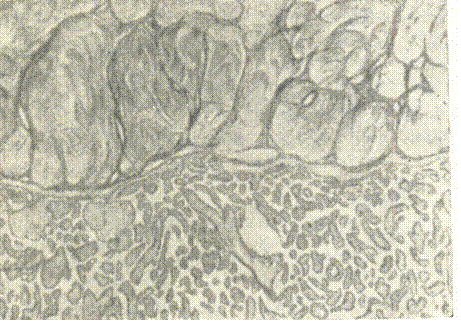
Fig. 191. Placenta adherent: underdeveloped (absent) spongy layer of the decidual membrane
Clinical signs (in case of partial adherence): just after the delivery of the fetus or 10-15 minutes after the delivery the external hemorrhage occurs. The blood is dark, with normal blood clots, no signs of separation of the afterbirth. The uterus is softened.
Treatment: catheterization of the bladder, manual removing of the afterbirth, massage of the uterus “on the fist”.
Fused placenta (total or partial). It is characterized by absence of spongy layer between the myometrium wall of the uterus and placental villi. It means the growing of the villi into the uterine wall. Three degrees are distinguished: 1) placental villi reach the myometrium (placenta accreta), 2) growing of the placental villi in between the myometrium fibres of the uterus (placenta increta), 3) penetration of the uterine wall with placental villi till the serous coat (placenta percreta). It may be partial and total (complete) too. There is no possibility of normal separation of the placenta. In partial fused placenta there is significant hemorrhage during the third stage of labor, because some placental parts are separated normally, while others — are not separated. The disrupted uterine vessels begin bleeding. The hemorrhage continues until the placenta is expelled from the uterus.
Clinical signs: in total fused placenta there is no hemorrhage during 30 (and more) minutes after the delivery of the fetus, no signs of placental (afterbirth) separation. In partial fused placenta there is bleeding, no signs of separation of the afterbirth. The differentiation between adherent placenta and fused placenta may be made only during manual control of the uterine cavity.
Treatment: In 15 minutes after the delivery of the fetus the intravenous infusion of the isotonic solution should be started, the bladder should be catheterized. Then the operation-hall and surgeons should be prepared. If no separation during the next 15 minutes takes place, a manual control of the uterine cavity should be performed. At fused placenta there is no possibility of its separation from the uterine wall and removing of afterbirth. This is accompanied by strengthening of bleeding and stratification of myometrium fibres. Thus, laparotomy and amputation of the uterus is indicated.
Defect of afterbirth. After the delivery of afterbirth it should be carefully examined. Lobes of the placenta may be left in the uterine cavity. Even a small portion of the placenta that may remain in the uterus after its delivery interferes with a normal contraction of the uterus. The disrupted vessels of the placental site therefore continue bleeding. Parts of the placenta may be retained in the uterus as a result of misconduct of the placental stage of labor and in connection with the adherent placenta. These complications always involve bleeding. The retention of fetal membranes does not present so serious danger, because membranes, as a rule, come out spontaneously. Nevertheless, at retention of more than 2/3 of membranes in the uterine cavity it is necessary to perform a manual revision of the uterus and removing of membranes and blood clots, with the purpose of prophylaxis of the described complications. Hemorrhage due to retention of parts of placenta in the uterine cavity may occur just after the delivery, or in the puerperal period; on the other hand it is one of the most frequent reasons of postpartum endometritis.
Clinical features. Bleeding begins soon after the delivery of the fetus or in a certain lapse of time (30-60 min). Within a short period of time the patient may lose from 500 to 1,000 ml (and over) of blood. The blood loss is sometimes as high as 1,500 ml. Hemorrhage is usually external; all blood freely flows out of the birth canal. But the mouth of womb may be closed by a spasm or a lobe of the placenta (or a clot of coagulated blood), and the blood will then accumulate inside the uterus. External bleeding is absent in such cases while the puerperium develops signs of acute anemia, the degree of which depends on the amount of the blood lost and on the health of the woman. Asthenic women and also women who had hypotension before labor develop an especially negative response to the loss of blood.
Developing anemia is characterized by pale skin and visible mucosa, decreased arterial pressure, accelerated pulse, vertigo, ear noise; if the blood loss is significant, the pulse becomes thready, the arterial pressure drops, and dyspnoea develops; the patient may die unless medical aid is given in due time.
Treatment includes manual separation of part of placenta remained in the uterine cavity. General anesthesia is obligatory for this intervention (given below).
Strangulation and retention of separated afterbirth in the uterine cavity (Fig. 192). Afterbirth becoming separated from the uterine wall can stay too long in the uterus at disturbance of its retractive power, at weakness of muscles of prelum abdominale, and also at spasm of internal os. The repletion of urinary bladder also can be the reason of retention of afterbirth in the uterus. The decrease of retractive power of uterus relies on numerous reasons and is the result of initial pathological changes, or is related to complications occurring during labor. At the same time the spasm of internal mouth of womb often occurs due to wrong conduct of placental stage of labor. So, belated administration of methylergometrine at head delivery can result in the spasm of internal os of the uterus. Every interference during a physiological course of placental stage of labor disturbs the separation of placenta, and is accompanied by the spasm of internal pharynx and restriction of afterbirth. Untimely and groundless attempts of expulsion of afterbirth, such as massage of the uterus, pulling by umbilical cord, lead to failure of afterbirth separation and expulsion and increase of hemorrhage. Placenta separated from the uterine wall and lying in the cavity of uterus becomes a foreign body that hinders in contraction of uterus and thrombosis of spiral vessels and leads to increase of blood loss.
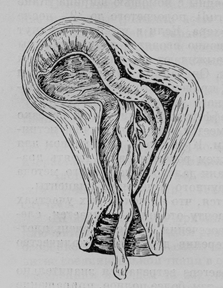
Fig. 192.Strangulation and retention of separated afterbirth in the uterine cavity
Clinical features. The signs of separation of placenta are positive, bleeding of different intensity takes place, there is no spontaneous expulsion of afterbirth.
Medical treatment. Catheterization of the urinary bladder is necessary, if it was not performed at once after delivery of the fetus. The use of external methods of expulsion of afterbirth separated from the uterine wall (Abuladze’s, Henter’s or Crede’s methods) should be attempted. To increase the uterine contraction it is necessary to perform local hypothermia of uterus (ice bag on the lower abdomen). If external methods of delivery of afterbirth are ineffective, it is necessary to give anesthesia, and perform the operation of manual removing of afterbirth, which is separated from the uterine wall.
Lacerations of the soft tissues of the birth canal. Lacerations of the cervix and deep lacerations of the vagina, perineum and external genitalia may be the cause of bleeding in the placental stage of labor and puerperium.
Bleeding starts immediately after delivery of the fetus or in a certain lapse of time; hemorrhage that begins during the placental stage sometimes persists in the puerperium. The amount of blood lost may be as high as 1,000 ml and over; acute anemia develops (the skin and mucosa become pallid, the pulse accelerates, the arterial pressure drops, vertigo develops, etc.)
Clinical features. Bleeding is continuous, with scarlet blood, begins at once after delivery of the fetus.
Treatment. It includes speculum examination of the birth canal, wound closure.
Basic Principles of Bleeding Arrest in the Third Period of Birth. The uterus may be contracted and bleeding stopped only after the uterus has been emptied. The placenta shall therefore be quickly removed from the uterus. If the placenta has separated, it can be extruded by external manipulations. If the placenta remains attached, the external manipulations may prove ineffective, and manual removal of the placenta is therefore recommended.
When bleeding starts, it is necessary to check immediately if the placenta is separated. If the signs of placental separation are positive, the placenta shall be removed by the Abuladze or Crede manoeuvre. In the absence of these signs an attempt should be made to extrude the placenta by the Crede manoeuvre (with anaesthesia). It sometimes fails because of the spasm of the internal cervix os; anesthesia removes the spasm and the placenta can thus be removed. If the Crede manoeuvre (with anaesthesia) proves ineffective, a recourse of manual separation of the placenta should be made.
If the signs of placental separation are negative, manual removing of the afterbirth is indicated at first.
Date added: 2022-12-25; views: 877;
